Excision of Cardiac Tumor (LA Myxoma) in a Severe Hypothyroidism Patient By Dr A. Sharda, Dr C.K. Ray Mohapatra, Dr A.K. Badmali
(Dept. of CTVS* and Dept of Cardiac Anaesthesia**), KIMS
Background
Primary cardiac tumors are rare, with an incidence of 1.38 per 100,000 people per year. Cardiac myxomas are noncancerous primary tumors of the heart and constitute about 50% of all primary heart tumors. Myxomas occur most often in patients aged 30 to 70, predominantly in women. About 75 to 85% of myxomas occur in the left atrium, 10 to 20% in the right atrium, and 5% in the ventricles. Although patients can be asymptomatic, symptoms may include dyspnea, angina, syncope, cough, vertigo, fatigue, fever and stroke. This case involves a patient with intermittent fevers, fatigue, and elevated C-reactive protein (CRP) that was eventually attributed to a myxoma. Hypothyroidism has generally been considered a contraindication to surgery. Thus, surgery in hypothyroid patients is associated with an increased risk of several minor peri-operative complications, which should be anticipated and preemptively managed in the course of their anesthetic and surgical care. Due to the emergency of the case, we operated the patient with high risk consent.
Case Presentation
A 55-year-old female patient was presented to the Cardiology Outpatient Department (OPD) with complaints of shortness of breath since six months (NYHA II) and one episode of syncopal attack three days back. The patient gave a typical history of breathlessness in the standing position (trepopnea), along with palpitations and generalized weakness. She was recently diagnosed with hypothyroidism. On examination, her vitals were stable. Systemic examination of the cardiovascular system (CVS) revealed systolic murmur and mid-diastolic murmur (tumor plop) over the apex; S1 was loud and there was an inspiratory split in S2.
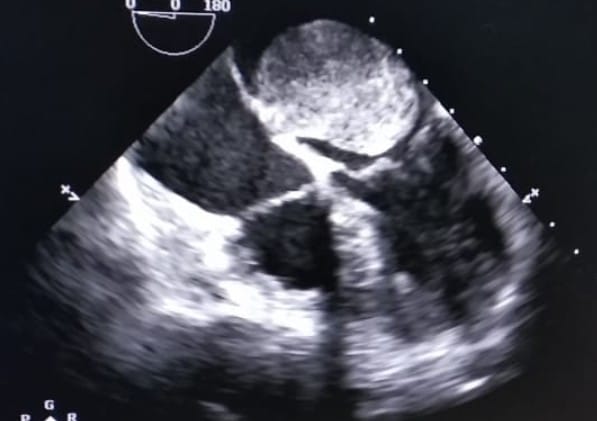
On investigating the patient, her blood count and liver and renal function tests were normal. Her TSH was 100 μIU/mL, FT3 1.96, FT 0.7. Electrocardiogram (ECG) and chest x-ray (CX-Ray) showed left atrial abnormality and right ventricular hypertrophy. Two-dimensional (2D) echocardiography (echo) revealed a large oval (5×4 cm size) globular mass in LA having a narrow stalk attaching to inferior IAS. Mass protruded to LV through the Mitral valve. Hence, the diagnosis of atrial myxoma was confirmed based on the history, clinical features, and noninvasive diagnostic tests such as 2D echo.
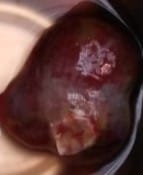
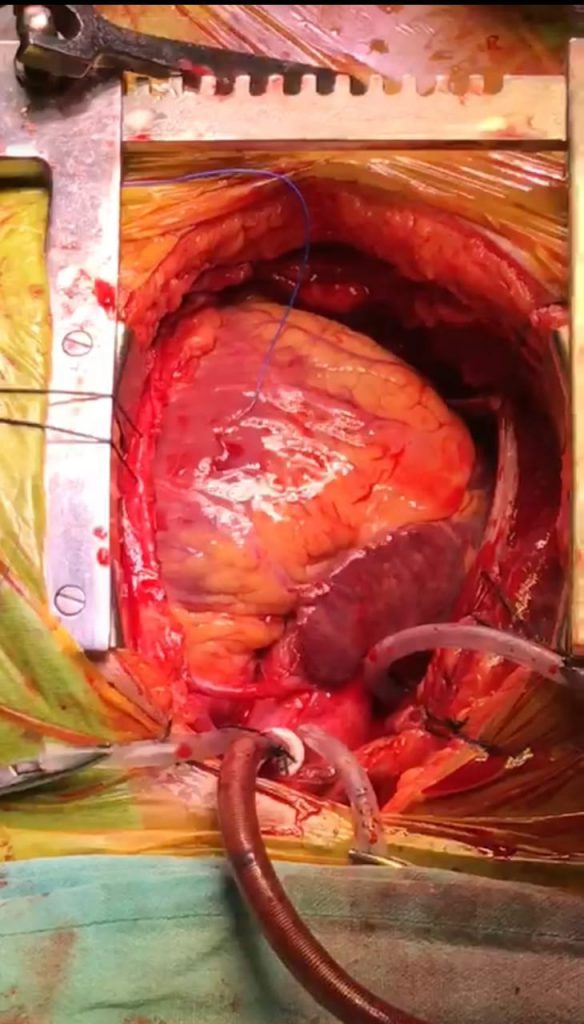
In view of a ball valve type of large myxoma with high risk of embolism and sudden cardiac death, she was taken up for surgery, despite her uncontrolled TSH, with informed high risk consent for surgery and post operative recovery. With 100 microgram of l thyroxine prior to the day of surgery, surgery was performed, the la myxoma was excised and the tumour was sent for histopathology. The HP report confirmed the tumor. After 1 month of follow up, the patient was doing well, and at present her breathlessness has improved and her auscultatory findings have also completely improved.